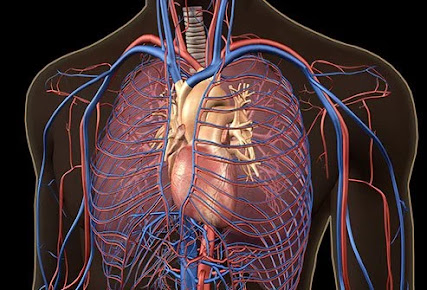
Pulmonary arterial hypertension (PAH) is a condition characterized by elevated blood pressure in the pulmonary arteries, leading to significant strain on the heart and impairing its ability to pump blood effectively. In normal circumstances, resting pulmonary artery systolic pressure typically ranges from 18 to 20 mmHg. However, in PAH, this pressure exceeds 25 mmHg at rest or rises above 30 mmHg with exercise, with a pulmonary capillary wedge pressure less than 15 mmHg as measured by right heart catheterization.
PAH can arise from a variety of underlying conditions affecting the pulmonary, cardiac, or systemic systems. Symptoms often manifest due to right ventricular failure or cor pulmonale, and may include dyspnea, fatigue, syncope, lower extremity edema, and atypical chest pain.
Furthermore, patients may initially experience exertional breathlessness, which can progress to exertional syncope or chest pain as the condition worsens.
Recent advancements in understanding the pathophysiology of PAH have led to targeted therapies that aim to alleviate symptoms, improve quality of life, and potentially slow disease progression. Early diagnosis and intervention are crucial in managing PAH and improving patient outcomes.
Understanding Pulmonary Arterial Hypertension
Showing posts with label definition. Show all posts
Showing posts with label definition. Show all posts
Thursday, April 25, 2024
Monday, April 08, 2024
Unveiling the Complexities of Peripheral Artery Disease (PAD)
Peripheral artery disease (PAD) is a relentless narrowing of arteries that crucially carry blood away from the heart, often suffocating vital organs and limbs. While it can afflict various regions, lower-extremity PAD, specifically impeding blood flow to the legs and feet, stands as the most prevalent form. This condition stems from atherosclerosis, a process characterized by the accumulation of fatty deposits and other substances within arteries, progressively constricting their lumens.
Unveiling the intricacies of PAD reveals its pervasive impact, extending beyond the lower extremities. Atherosclerosis, the culprit behind PAD, indiscriminately encroaches upon arteries throughout the body, including those vital for heart, brain, arm, leg, pelvic, and renal function. Such widespread arterial blockage underscores the urgent need for early diagnosis to mitigate grave secondary vascular events like acute myocardial infarction (AMI) or stroke.
Swift identification of occlusive arterial disease hinges upon noninvasive assessments, with the ankle-brachial index (ABI) emerging as a cornerstone diagnostic tool. Not only does ABI discern the presence of arterial compromise, but it also furnishes invaluable insights into the prognosis of affected limbs, prognosticating the likelihood of AMI during follow-up.
PAD's insidious nature often conceals its presence in its nascent stages, camouflaging its progression until symptomatic manifestations emerge. These symptoms, such as intermittent claudication and rest pain, serve as ominous harbingers of advancing disease. Intermittent claudication, characterized by muscle aches or cramps following exertion, abates with rest but underscores compromised arterial circulation. Conversely, rest pain, an affliction haunting patients even in repose, signals critical limb ischemia—a dire consequence of oxygen deprivation to tissues. Such ischemic insults perpetuate a vicious cycle, hindering wound healing and fostering ulceration and gangrene. As PAD advances unabated, ulceration festers and gangrene ensues, precipitating the ominous specter of limb loss and necessitating amputation as a last resort.
In conclusion, the labyrinthine nature of PAD underscores the imperative of vigilance in diagnosis and management. Early detection facilitated by ABI empowers clinicians to intervene preemptively, averting catastrophic vascular sequelae. By unraveling PAD's enigma and prioritizing comprehensive care, we can strive towards preserving both life and limb in the face of this formidable arterial adversary.
Unveiling the Complexities of Peripheral Artery Disease (PAD)
Unveiling the intricacies of PAD reveals its pervasive impact, extending beyond the lower extremities. Atherosclerosis, the culprit behind PAD, indiscriminately encroaches upon arteries throughout the body, including those vital for heart, brain, arm, leg, pelvic, and renal function. Such widespread arterial blockage underscores the urgent need for early diagnosis to mitigate grave secondary vascular events like acute myocardial infarction (AMI) or stroke.
Swift identification of occlusive arterial disease hinges upon noninvasive assessments, with the ankle-brachial index (ABI) emerging as a cornerstone diagnostic tool. Not only does ABI discern the presence of arterial compromise, but it also furnishes invaluable insights into the prognosis of affected limbs, prognosticating the likelihood of AMI during follow-up.
PAD's insidious nature often conceals its presence in its nascent stages, camouflaging its progression until symptomatic manifestations emerge. These symptoms, such as intermittent claudication and rest pain, serve as ominous harbingers of advancing disease. Intermittent claudication, characterized by muscle aches or cramps following exertion, abates with rest but underscores compromised arterial circulation. Conversely, rest pain, an affliction haunting patients even in repose, signals critical limb ischemia—a dire consequence of oxygen deprivation to tissues. Such ischemic insults perpetuate a vicious cycle, hindering wound healing and fostering ulceration and gangrene. As PAD advances unabated, ulceration festers and gangrene ensues, precipitating the ominous specter of limb loss and necessitating amputation as a last resort.
In conclusion, the labyrinthine nature of PAD underscores the imperative of vigilance in diagnosis and management. Early detection facilitated by ABI empowers clinicians to intervene preemptively, averting catastrophic vascular sequelae. By unraveling PAD's enigma and prioritizing comprehensive care, we can strive towards preserving both life and limb in the face of this formidable arterial adversary.
Unveiling the Complexities of Peripheral Artery Disease (PAD)
Wednesday, July 27, 2022
Pulmonary embolism
Pulmonary embolism is a blockage that developed when a blood clot gets caught in one of the arteries that go from the heart to the lungs. The clot blocks the normal flow of blood.
A blood clot that forms in a blood vessel in one area of the body, breaks off, and travels to another area of the body in the blood is called an embolus. An embolus can lodge itself in a blood vessel. This can block the blood supply to a particular organ.
Pulmonary embolism restricts blood flow to the lungs, lowers oxygen levels in the lungs and increases blood pressure in the pulmonary arteries.
In most cases, pulmonary embolism is caused by blood clots that travel to the lungs from deep veins in the legs or, rarely, from veins in other parts of the body (deep vein thrombosis). These clots develop when the blood can’t flow freely through the legs because human body is still for a long time, say during a long flight or drive.
Common signs and symptoms include:
*Shortness of breath
*Chest pain
*Cough
*Difficulty breathing
*Panting
*Fast heartbeat
If left untreated, acute pulmonary embolism is associated with a mortality rate as high as 30%.
Pulmonary embolism is often difficult to diagnose because the signs and symptoms of pulmonary embolism are a lot like those of many other conditions and diseases. Imaging tests and blood tests are used to look for a pulmonary embolism.
Pulmonary embolism
A blood clot that forms in a blood vessel in one area of the body, breaks off, and travels to another area of the body in the blood is called an embolus. An embolus can lodge itself in a blood vessel. This can block the blood supply to a particular organ.
Pulmonary embolism restricts blood flow to the lungs, lowers oxygen levels in the lungs and increases blood pressure in the pulmonary arteries.
In most cases, pulmonary embolism is caused by blood clots that travel to the lungs from deep veins in the legs or, rarely, from veins in other parts of the body (deep vein thrombosis). These clots develop when the blood can’t flow freely through the legs because human body is still for a long time, say during a long flight or drive.
Common signs and symptoms include:
*Shortness of breath
*Chest pain
*Cough
*Difficulty breathing
*Panting
*Fast heartbeat
If left untreated, acute pulmonary embolism is associated with a mortality rate as high as 30%.
Pulmonary embolism is often difficult to diagnose because the signs and symptoms of pulmonary embolism are a lot like those of many other conditions and diseases. Imaging tests and blood tests are used to look for a pulmonary embolism.
Pulmonary embolism
Tuesday, July 05, 2022
What is hypertensive heart disease?
Hypertension remains a major public health problem associated with considerable morbidity and mortality. It’s the leading cause of death from high blood pressure. Hypertensive heart disease encompasses anatomical changes and altered physiology of heart muscle, coronary arteries, and great vessels.
Hypertensive heart disease refers to a constellation of changes in the left ventricle, left atrium and coronary arteries as a result of chronic blood pressure elevation. It’s a group of medical problems ― like heart failure and conduction arrhythmias ― that can happen when the person doesn’t control his high blood pressure (hypertension).
Essential hypertension accounts for 90% of cases of hypertension in adults. Secondary causes of hypertension account for the remaining 10% of cases of chronically elevated BP.
Hypertension increases the workload on the heart inducing structural and functional changes in the myocardium. These changes include hypertrophy of the left ventricle, which can progress to heart failure.
Clinically, hypertensive heart disease is characterized by the presence of left ventricular hypertrophy (LVH) in the absence of a cause other than arterial hypertension.
The main risk factor for hypertensive heart disease is high blood pressure. The risk increases if the person overweight, not exercise enough, smoking, eating food high in fat and cholesterol. Chronic high blood pressure (higher than 120/80 mmHg) causes hypertensive heart disease. As people get older and continue to have high blood pressure, their risk of heart disease increases.
Hypertensive heart disease can cause serious health problems. Hypertensive heart disease can lead to either diastolic heart failure, systolic failure or a combination of the two. Such patients are at a higher risk for developing acute complications such as decompensated heart failure, acute coronary syndrome or sudden cardiac death.
The types of hypertensive heart disease include:
*Narrowing of the arteries
*Thickening and enlargement of the heart
What is hypertensive heart disease?
Hypertensive heart disease refers to a constellation of changes in the left ventricle, left atrium and coronary arteries as a result of chronic blood pressure elevation. It’s a group of medical problems ― like heart failure and conduction arrhythmias ― that can happen when the person doesn’t control his high blood pressure (hypertension).
Essential hypertension accounts for 90% of cases of hypertension in adults. Secondary causes of hypertension account for the remaining 10% of cases of chronically elevated BP.
Hypertension increases the workload on the heart inducing structural and functional changes in the myocardium. These changes include hypertrophy of the left ventricle, which can progress to heart failure.
Clinically, hypertensive heart disease is characterized by the presence of left ventricular hypertrophy (LVH) in the absence of a cause other than arterial hypertension.
The main risk factor for hypertensive heart disease is high blood pressure. The risk increases if the person overweight, not exercise enough, smoking, eating food high in fat and cholesterol. Chronic high blood pressure (higher than 120/80 mmHg) causes hypertensive heart disease. As people get older and continue to have high blood pressure, their risk of heart disease increases.
Hypertensive heart disease can cause serious health problems. Hypertensive heart disease can lead to either diastolic heart failure, systolic failure or a combination of the two. Such patients are at a higher risk for developing acute complications such as decompensated heart failure, acute coronary syndrome or sudden cardiac death.
The types of hypertensive heart disease include:
*Narrowing of the arteries
*Thickening and enlargement of the heart
What is hypertensive heart disease?
Friday, July 09, 2021
Hyperlipidemia
Hyperlipidemia is a family of disorders that are characterized by abnormally high levels of lipids in the blood. This condition is also called hypercholesterolemia or hyperlipoproteinemia. It is a very common disorder, especially in the Western hemisphere, but also throughout the world.
While fats play a vital role in the body’s metabolic processes, high blood levels of fats increase the risk of coronary heart disease (CHD). Hyperlipidemia is a major cause of atherosclerosis and atherosclerosis related conditions like coronary heart disease (CHD), ischemic cerebrovascular disease, peripheral vascular disease and pancreatitis.
The increase in lipids like low density lipoproteins (LDL), cholesterol (esters derivatives) and triglycerides are mainly responsible for this condition. Cholesterol, saturated fat, trans fat in the following food may raise the lipid level in blood:
• Dairy products.
• Ice cream pastries.
• Fried and junk foods.
• Meat
Several other causes of hyperlipidemia
• Obesity.
• Genetic or inheritance.
• Smoking.
Hyperlipidemia can be classified on the basis of lipid type:
*Hypercholesterolemia-In this the level of cholesterol is elevated.
*Hypertriglyceridemia-It is defined as an elevated level of triglycerides.
Hyperlipidemia disease has afflicted humankind since antiquity. Hyperlipidemia is the leading risk factor for cardiovascular diseases. Cholesterol and triglycerides together make it difficult for blood to pass by narrowing the blood vessels.
Complications of hyperlipidemia:
*Atherosclerosis
*Coronary Artery Disease
*Myocardial Infarction
*Angina Pectoris
*Ischemic stroke or Cerebrovascular Accident
Hyperlipidemia
While fats play a vital role in the body’s metabolic processes, high blood levels of fats increase the risk of coronary heart disease (CHD). Hyperlipidemia is a major cause of atherosclerosis and atherosclerosis related conditions like coronary heart disease (CHD), ischemic cerebrovascular disease, peripheral vascular disease and pancreatitis.
The increase in lipids like low density lipoproteins (LDL), cholesterol (esters derivatives) and triglycerides are mainly responsible for this condition. Cholesterol, saturated fat, trans fat in the following food may raise the lipid level in blood:
• Dairy products.
• Ice cream pastries.
• Fried and junk foods.
• Meat
Several other causes of hyperlipidemia
• Obesity.
• Genetic or inheritance.
• Smoking.
Hyperlipidemia can be classified on the basis of lipid type:
*Hypercholesterolemia-In this the level of cholesterol is elevated.
*Hypertriglyceridemia-It is defined as an elevated level of triglycerides.
Hyperlipidemia disease has afflicted humankind since antiquity. Hyperlipidemia is the leading risk factor for cardiovascular diseases. Cholesterol and triglycerides together make it difficult for blood to pass by narrowing the blood vessels.
Complications of hyperlipidemia:
*Atherosclerosis
*Coronary Artery Disease
*Myocardial Infarction
*Angina Pectoris
*Ischemic stroke or Cerebrovascular Accident
Hyperlipidemia
Monday, April 05, 2021
What is hypertensive heart disease?
Hypertension can lead to hypertensive heart disease, which is a condition that represents an important underlying mechanism for the occurrence of blood pressure-related CVD morbidity and mortality.
Hypertensive heart disease encompasses anatomical changes and altered physiology of heart muscle, coronary arteries, and great vessels.
Hypertensive heart disease is a constellation of abnormalities that includes left ventricular hypertrophy (LVH), systolic and diastolic dysfunction, and their clinical manifestations including arrhythmias and symptomatic heart failure.
Hypertensive heart disease results from chronic high blood pressure. Hypertension can be defined as blood pressure as a systolic blood pressure higher than 120 mm Hg or a diastolic pressure more than 80mm Hg. The risk of cardiovascular mortality doubles for every 20mmHg systolic and 10mmHg diastolic pressure increase over a baseline blood pressure of 115/75.
Clinically, hypertensive heart disease is characterized by the presence of left ventricular hypertrophy (LVH) in the absence of a cause other than arterial hypertension.
Hypertensive individuals with hypertensive heart disease are more prone to myocardial infarction, congestive heart failure, stroke, and sudden death then persons with hypertension alone.
The main risk factor for hypertensive heart disease is high blood pressure. The risk increases if the person overweight, not exercise enough, smoking, eating food high in fat and cholesterol.
Types of hypertensive heart disease:
*Narrowing of the arteries
*Thickening and enlargement of the heart
What is hypertensive heart disease?
Hypertensive heart disease encompasses anatomical changes and altered physiology of heart muscle, coronary arteries, and great vessels.
Hypertensive heart disease is a constellation of abnormalities that includes left ventricular hypertrophy (LVH), systolic and diastolic dysfunction, and their clinical manifestations including arrhythmias and symptomatic heart failure.
Hypertensive heart disease results from chronic high blood pressure. Hypertension can be defined as blood pressure as a systolic blood pressure higher than 120 mm Hg or a diastolic pressure more than 80mm Hg. The risk of cardiovascular mortality doubles for every 20mmHg systolic and 10mmHg diastolic pressure increase over a baseline blood pressure of 115/75.
Clinically, hypertensive heart disease is characterized by the presence of left ventricular hypertrophy (LVH) in the absence of a cause other than arterial hypertension.
Hypertensive individuals with hypertensive heart disease are more prone to myocardial infarction, congestive heart failure, stroke, and sudden death then persons with hypertension alone.
The main risk factor for hypertensive heart disease is high blood pressure. The risk increases if the person overweight, not exercise enough, smoking, eating food high in fat and cholesterol.
Types of hypertensive heart disease:
*Narrowing of the arteries
*Thickening and enlargement of the heart
What is hypertensive heart disease?
Wednesday, October 07, 2020
Cardiac Hypertrophy
Cardiac hypertrophy is defined as an abnormal increase in heart muscle mass, reflects a response of myocardium to mechanical stress and various stimuli.
Hypertrophy is derived from the Greek hyper, meaning over, and trophy, meaning abnormal enlargement of a part of organ or excessive growth. Hypertrophy is widely believed to be an adaptive response to increased workload or excessive training. By undergoing hypertrophy, ventricular wall stress remains constant at higher intraventricular pressures.
The primary molecular cause of enlargement of the heart is hypertrophy of myocytes (i.e., enlargement of existing cells, without an increase in the number of cells).
At a molecular level, it has been shown to be a dynamic process during the progression of long-standing hypertrophy to eventual heart failure.
First type, eccentric hypertrophy, in which the precipitating stress is volume overload, is characterized by increased heart-wall thickness and ventricular dilation but addition of sarcomere in series. It is more commonly associated with endurance exercise training (e.g., swimming, cycling, and running) pregnancy, and volume overload.
Second one, concentric hypertrophy, in which the imposed stress is pressure overload, is characterized by an increase in wall thickness with the deposition of new sarcomeres, but the chamber radius may not change. It is most often the result of chronic pressure overload, but is possible to a minor degree with isometric physical training such as weight training, weight and hammer throwing, wrestling and bodybuilding.
Cardiac Hypertrophy
Note: Sarcomere is the basic contractile unit of muscle fiber. Each sarcomere is composed of two main protein filaments—actin and myosin
Hypertrophy is derived from the Greek hyper, meaning over, and trophy, meaning abnormal enlargement of a part of organ or excessive growth. Hypertrophy is widely believed to be an adaptive response to increased workload or excessive training. By undergoing hypertrophy, ventricular wall stress remains constant at higher intraventricular pressures.
The primary molecular cause of enlargement of the heart is hypertrophy of myocytes (i.e., enlargement of existing cells, without an increase in the number of cells).
At a molecular level, it has been shown to be a dynamic process during the progression of long-standing hypertrophy to eventual heart failure.
First type, eccentric hypertrophy, in which the precipitating stress is volume overload, is characterized by increased heart-wall thickness and ventricular dilation but addition of sarcomere in series. It is more commonly associated with endurance exercise training (e.g., swimming, cycling, and running) pregnancy, and volume overload.
Second one, concentric hypertrophy, in which the imposed stress is pressure overload, is characterized by an increase in wall thickness with the deposition of new sarcomeres, but the chamber radius may not change. It is most often the result of chronic pressure overload, but is possible to a minor degree with isometric physical training such as weight training, weight and hammer throwing, wrestling and bodybuilding.
Cardiac Hypertrophy
Note: Sarcomere is the basic contractile unit of muscle fiber. Each sarcomere is composed of two main protein filaments—actin and myosin
Wednesday, March 21, 2018
Takayasu's disease
Takayasu's disease, also known as Takaysu's arteritis, is a rare and chronic inflammatory vascular disorder that primarily affects the aorta and its main branches as well as the pulmonary arteries and results in absent limb pulses and retinopathy. Features include cerebrovascular insufficiency (fainting, dizziness) and reduce peripheral pulses.
Acute progression of the disease can lead to destruction of the arterial media, formation of aneurysms, or arterial rupture. The first description of Takayasu’s disease was given in 1830 by Rokushu Yamamoto. He described a 45-year old man with fever, pulselessness, loss of weight, and breathlessness, who died in his 11th year of follow-up.
Takayasu's disease predominantly affects Asian females with an overall male-to-female ratio of 1 to 8.5. In the majority of cases, the age of onset is typically under 40, especially between 10 and 20 years of age.
Takayasu’s arteritis emerges in response to aortic burden, in addition to involvement of the aorta’s main branches, resulting in systemic vascular and potential immune response.
Because patients with early Takayasu’s arteritis may have nonspecific symptoms and because the disease is so rare, a doctor may not suspect Takayasu’s arteritis until symptoms of arterial narrowing develop. This could be months or even years into the course of the illness.
Takayasu's disease
Acute progression of the disease can lead to destruction of the arterial media, formation of aneurysms, or arterial rupture. The first description of Takayasu’s disease was given in 1830 by Rokushu Yamamoto. He described a 45-year old man with fever, pulselessness, loss of weight, and breathlessness, who died in his 11th year of follow-up.
Takayasu's disease predominantly affects Asian females with an overall male-to-female ratio of 1 to 8.5. In the majority of cases, the age of onset is typically under 40, especially between 10 and 20 years of age.
Takayasu’s arteritis emerges in response to aortic burden, in addition to involvement of the aorta’s main branches, resulting in systemic vascular and potential immune response.
Because patients with early Takayasu’s arteritis may have nonspecific symptoms and because the disease is so rare, a doctor may not suspect Takayasu’s arteritis until symptoms of arterial narrowing develop. This could be months or even years into the course of the illness.
Takayasu's disease
Friday, October 13, 2017
Gastrocardiac syndrome
Gastrocardiac syndrome is the most common cause of noncardiac substernal chest pain in the elderly. It is common in Asia and he been described in Germany for some years as “Roemheld’s Syndrome.”
Other names for this condition include Bergmann's diaphragmatic hernia syndrome, von Bergmann's syndrome, epiphrenal syndrome, gastrocardial symptom, complex, hiatus hernia syndrome, paraesophageal hernia syndrome and sliding diaphragmatic hernia syndrome.
It refers to alteration in the heart rhythm caused by reflux of stomach juice. This condition may either congenital or acquired. When congenital, it is linked to autosomal recessive or x-linked inheritance. Acquired causes include being overweight and Heliobacter phylori infection.
Diagnosis gastrocardiac syndrome based on the exclusion of heart disease (coronary artery disease, arrhythmias), other diseases mediastinal organs (mediastinitis, aneurysm thoracic aorta), as well as identifying the pathology of the gastrointestinal tract, which can cause seizures (hiatal hernia, ulcer ulcer, gastric cancer, esophageal).
There are three types of gastrocardiac syndromes:
*Kardialgichesky – the main clinical and functional manifestations of syndrome are pain in the heart occurring during physical exertion, accompanied by shortness of breath, palpitations. Triglycerides were significantly higher than in other gastrocardiac syndromes.
*Arrhythmic – Systolic and diastolic pressure was significantly higher compared with patients of other groups.
*Dystonic – The phenomena of false angina accompanied by marked autonomic dysfunction (sweating, increased nervous irritability, sleep disturbance)
Gastrocardiac syndrome
Other names for this condition include Bergmann's diaphragmatic hernia syndrome, von Bergmann's syndrome, epiphrenal syndrome, gastrocardial symptom, complex, hiatus hernia syndrome, paraesophageal hernia syndrome and sliding diaphragmatic hernia syndrome.
It refers to alteration in the heart rhythm caused by reflux of stomach juice. This condition may either congenital or acquired. When congenital, it is linked to autosomal recessive or x-linked inheritance. Acquired causes include being overweight and Heliobacter phylori infection.
Diagnosis gastrocardiac syndrome based on the exclusion of heart disease (coronary artery disease, arrhythmias), other diseases mediastinal organs (mediastinitis, aneurysm thoracic aorta), as well as identifying the pathology of the gastrointestinal tract, which can cause seizures (hiatal hernia, ulcer ulcer, gastric cancer, esophageal).
There are three types of gastrocardiac syndromes:
*Kardialgichesky – the main clinical and functional manifestations of syndrome are pain in the heart occurring during physical exertion, accompanied by shortness of breath, palpitations. Triglycerides were significantly higher than in other gastrocardiac syndromes.
*Arrhythmic – Systolic and diastolic pressure was significantly higher compared with patients of other groups.
*Dystonic – The phenomena of false angina accompanied by marked autonomic dysfunction (sweating, increased nervous irritability, sleep disturbance)
Gastrocardiac syndrome
Sunday, February 05, 2017
Cardiac arrhythmia
Cardiac rhythms under physiological conditions are set by pacemakers cells that are normally capable of developing spontaneous depolarization and are responsible for generating the cardiac rhythm.
Cardiac rhythm that deviates from the normal automatic rhythm is referred to as cardiac arrhythmia, often manifested in the form of tachycardia. Cardiac arrhythmia is one of the leading causes of death in many countries worldwide. What is cardiac arrhythmia? Cardiac arrhythmia is a term used to refer to any condition that disrupts the normal electrical activity of the heart which can lead to sudden cardiac death.
Arrhythmias can affect the heart rate causing irregular rhythms, such as slow or fats heartbeat.
In United States, fatalities due to cardiac arrhythmia mostly caused by cardiopulmonary failure, trauma, metabolic imbalance such as renal failure or diabetes or a systemic illness.
Some arrhythmias clearly produce serious hemodynamic compromise that can be fatal, but some cause no clinically evident problems. Other arrhythmias may portend increased risk for sudden arrhythmia detach.
Cardiac arrhythmia
Cardiac rhythm that deviates from the normal automatic rhythm is referred to as cardiac arrhythmia, often manifested in the form of tachycardia. Cardiac arrhythmia is one of the leading causes of death in many countries worldwide. What is cardiac arrhythmia? Cardiac arrhythmia is a term used to refer to any condition that disrupts the normal electrical activity of the heart which can lead to sudden cardiac death.
Arrhythmias can affect the heart rate causing irregular rhythms, such as slow or fats heartbeat.
In United States, fatalities due to cardiac arrhythmia mostly caused by cardiopulmonary failure, trauma, metabolic imbalance such as renal failure or diabetes or a systemic illness.
Some arrhythmias clearly produce serious hemodynamic compromise that can be fatal, but some cause no clinically evident problems. Other arrhythmias may portend increased risk for sudden arrhythmia detach.
Cardiac arrhythmia
Wednesday, December 07, 2016
Cardiomyopathy
Cardiomyopathy refers to any disease that affects the heart muscle, this diminishing cardiac performance. It is a rare form of heart disease that affects only the heart muscle.
The term cardiomyopathy is derived from the word cardio, the heart, and myopathy, which indicates a weakness or disturbance of the muscle.
Cardiomyopathy occurs in three major types: dilated congestive, hypertrophic and restrictive. Dilated congestive, the most common, is the form seen in children and occur in autosomal dominant, X-linked and sporadic forms.
The heart loses its ability to pump blood and in some instances, heart rhythm is disturb, leading to irregular heartbeats or arrhythmias.
The causes of cardiomyopathy are somewhat reflected in their names. Primary cardiomyopathy refers to cardiomyopathy of unknown etiology. Hypertrophic cardiomyopathy is a specific type of primary cardiomyopathy in which the cause in uncertain. Hypertrophic cardiomyopathy is found throughout the world with a prevalence in North America of 0.2%.
Secondary cardiomyopathy is cardiomyopathy due to a well-defined systemic disease. For instance, alcoholic cardiomyopathy, as to its name implies, is due to long standing alcohol abuse.
Cardiomyopathy
The term cardiomyopathy is derived from the word cardio, the heart, and myopathy, which indicates a weakness or disturbance of the muscle.
Cardiomyopathy occurs in three major types: dilated congestive, hypertrophic and restrictive. Dilated congestive, the most common, is the form seen in children and occur in autosomal dominant, X-linked and sporadic forms.
The heart loses its ability to pump blood and in some instances, heart rhythm is disturb, leading to irregular heartbeats or arrhythmias.
The causes of cardiomyopathy are somewhat reflected in their names. Primary cardiomyopathy refers to cardiomyopathy of unknown etiology. Hypertrophic cardiomyopathy is a specific type of primary cardiomyopathy in which the cause in uncertain. Hypertrophic cardiomyopathy is found throughout the world with a prevalence in North America of 0.2%.
Secondary cardiomyopathy is cardiomyopathy due to a well-defined systemic disease. For instance, alcoholic cardiomyopathy, as to its name implies, is due to long standing alcohol abuse.
Cardiomyopathy
Thursday, June 16, 2016
Cerebral arteriography
In 1926 Portuguese physician Caetano de Egas Moniz invented cerebral arteriography, x-ray of the skull after introducing a contrast medium into both carotid and arteries.
Egas mounted his camera in the ‘radio-carousel’ invented by his colleague Jose Pereira Caldas to get a large series of angiograms in rapid succession. He was awarded a Nobel Prize in Medicine in 1949 for developing the first psychosurgery procedure.
Cerebral arteriography or angiography is a procedure by which the intracranial and extracranial head and neck circulation is evaluated.
It entails the placement of a catheter selectively into extracranial cerebral vessels using fluoroscopic guidance followed by contrast injection and image acquisition to delineate anatomy and abnormalities.
Conventional cerebral angiography is recommended for all patients with spontaneous intracerebral hemorrhage, expect for those older than 45 years with pre-existing hypertension in thalamic, putaminal or posterior fossa hemorrhage. Cerebral angiography can detect arterial and venous stenosis, vascular malformations or tumors.
Cerebral arteriography
Egas mounted his camera in the ‘radio-carousel’ invented by his colleague Jose Pereira Caldas to get a large series of angiograms in rapid succession. He was awarded a Nobel Prize in Medicine in 1949 for developing the first psychosurgery procedure.
Cerebral arteriography or angiography is a procedure by which the intracranial and extracranial head and neck circulation is evaluated.
It entails the placement of a catheter selectively into extracranial cerebral vessels using fluoroscopic guidance followed by contrast injection and image acquisition to delineate anatomy and abnormalities.
Conventional cerebral angiography is recommended for all patients with spontaneous intracerebral hemorrhage, expect for those older than 45 years with pre-existing hypertension in thalamic, putaminal or posterior fossa hemorrhage. Cerebral angiography can detect arterial and venous stenosis, vascular malformations or tumors.
Cerebral arteriography
Sunday, November 08, 2015
Cerebrovascular disease
Cerebral vascular disorders are characterized by sudden neurologic deficits resulting from ischemia or hemorrhagic events.
Cerebrovascular disease is one of the most common neurologic diseases, with a relatively high cases fatality ratio and a substantial personal, familial and social impact among the survivors.
Cerebrovascular disease is the third leading cause of death and the leading cause of disability in the United States. Many different cerebrovascular diseases may cause cognitive decline and dementia, including stroke, silent infarcts, ischemic white matter lesions, hereditary cerebral hemorrhage with amyloidosis, granular cortical atrophy, hypertensive encephalopathy, cerebral amyloid angiopathy and cerebral vasculitis.
The major risk factors for the development of cerebrovascular disease are hypertension and diabetes.
Other risk factors include atherosclerosis, inflammatory processes, dissecting aneurysm, disorders affecting the myocardium, congestive heart failure, polycythemia, cigarette smoking, use of oral contraceptives and postpartum infection.
Cerebrovascular disease
Cerebrovascular disease is one of the most common neurologic diseases, with a relatively high cases fatality ratio and a substantial personal, familial and social impact among the survivors.
Cerebrovascular disease is the third leading cause of death and the leading cause of disability in the United States. Many different cerebrovascular diseases may cause cognitive decline and dementia, including stroke, silent infarcts, ischemic white matter lesions, hereditary cerebral hemorrhage with amyloidosis, granular cortical atrophy, hypertensive encephalopathy, cerebral amyloid angiopathy and cerebral vasculitis.
The major risk factors for the development of cerebrovascular disease are hypertension and diabetes.
Other risk factors include atherosclerosis, inflammatory processes, dissecting aneurysm, disorders affecting the myocardium, congestive heart failure, polycythemia, cigarette smoking, use of oral contraceptives and postpartum infection.
Cerebrovascular disease
Monday, June 15, 2015
Hypertensive heart disease
Hypertension is a powerful predictor of cardiovascular mortality and death from all causes. It is a major risk factor for the development of systolic heart failure as well as heart failure in the setting of preserved left ventricular function.
Hypertensive heart disease can be defined as the response of the heart to the afterload imposed on the left ventricle by the progressively increasing arterial pressure and total peripheral resistance.
Severe hypertension may directly damage arterioles and cause atherosclerosis. High blood pressure is also a risk for stroke.
The risk of cardiovascular events is increased two or three times in men and women with hypertension. It is estimated that 14% deaths from coronary heart disease in men and 12% of deaths from coronary heart disease in women are due to hypertension.
Hypertensive heart disease is characterized by increased left ventricular mass leading to left ventricular hypertrophy in the absence of aortic stenosis or hypertrophic cardiomyopathy. Other manifestations include diastolic dysfunction and microvascular changes that cause coronary blood flow abnormalities.
Left ventricular hypertrophy increases the rletaove risk for amrtlaity by twofold in subjects with coronary artery disease and by four fold in those with normal epicardial coronary arteries.
In the development of hypertensive heart disease, myocyte hypertrophy is also associated with apoptosis, collagen deposition, a ventricular fibrosis, with as impairment of coronary hemodynamics as well, thus profoundly influencing functional properties of the left ventricle.
Hypertensive heart disease
Hypertensive heart disease can be defined as the response of the heart to the afterload imposed on the left ventricle by the progressively increasing arterial pressure and total peripheral resistance.
Severe hypertension may directly damage arterioles and cause atherosclerosis. High blood pressure is also a risk for stroke.
The risk of cardiovascular events is increased two or three times in men and women with hypertension. It is estimated that 14% deaths from coronary heart disease in men and 12% of deaths from coronary heart disease in women are due to hypertension.
Hypertensive heart disease is characterized by increased left ventricular mass leading to left ventricular hypertrophy in the absence of aortic stenosis or hypertrophic cardiomyopathy. Other manifestations include diastolic dysfunction and microvascular changes that cause coronary blood flow abnormalities.
Left ventricular hypertrophy increases the rletaove risk for amrtlaity by twofold in subjects with coronary artery disease and by four fold in those with normal epicardial coronary arteries.
In the development of hypertensive heart disease, myocyte hypertrophy is also associated with apoptosis, collagen deposition, a ventricular fibrosis, with as impairment of coronary hemodynamics as well, thus profoundly influencing functional properties of the left ventricle.
Hypertensive heart disease
Monday, April 20, 2015
What is meant by blood pressure?
Human body needs the nutrients and oxygen from blood. Blood is pumped from the heart and it travels around the body delivering oxygen and nutrients to the organs of the body and returns to the heart ready to be pumped back out again.
Blood pressure is needed so that the blood can travel from heart to other organs and muscles.
An adult has around five liters of blood that circulates around the body approximately once every minute. Blood pressure is the force of the blood pushing against the walls of those arteries.
Each times the heart beats (about 60-70 times a minute at rest), it pumps out blood into the arteries. Blood pressure monitoring is an important indicator of a wearer’s cardiovascular status.
Many devices allow blood pressure to be measured by manual or digital sphygmomanometer systems that utilize an inflatable cuff applied to a person’s arm.
The blood pressure is at its greatest when the heart contracts and is pumping the blood. This is called systolic pressure.
When the heart is at rest, in between beats, the blood pressure falls. This is the diastolic pressure.
When blood pressure stays too high for too long, it can damage the blood vessels. Organs such as kidneys, heart, brain and eyes can be affected.
High blood pressure is the leading risk factor for heart failure. It also increases the risk later for atherosclerosis or hardening of the arteries.
What is meant by blood pressure?
Blood pressure is needed so that the blood can travel from heart to other organs and muscles.
An adult has around five liters of blood that circulates around the body approximately once every minute. Blood pressure is the force of the blood pushing against the walls of those arteries.
Each times the heart beats (about 60-70 times a minute at rest), it pumps out blood into the arteries. Blood pressure monitoring is an important indicator of a wearer’s cardiovascular status.
Many devices allow blood pressure to be measured by manual or digital sphygmomanometer systems that utilize an inflatable cuff applied to a person’s arm.
The blood pressure is at its greatest when the heart contracts and is pumping the blood. This is called systolic pressure.
When the heart is at rest, in between beats, the blood pressure falls. This is the diastolic pressure.
When blood pressure stays too high for too long, it can damage the blood vessels. Organs such as kidneys, heart, brain and eyes can be affected.
High blood pressure is the leading risk factor for heart failure. It also increases the risk later for atherosclerosis or hardening of the arteries.
What is meant by blood pressure?
Sunday, December 14, 2014
Pulmonary stenosis
The majority of pulmonary stenosis are conginetal. It cause by abnormal formation of the pulmonary valve leaflets during fetal cardiac development. Rarely, rheumatic heart disease, malignant carcinoid, or extrinsic compression by a tumor or sinus of valsalva aneurysm may lead to pulmonary stenosis.
Pulmonary stenosis can be valvular, subvalvular or supravalvular. Valvular pulmonary stenosis is the most common, accounting for 90% cases.
Subvalvular pulmonary stenosis can occur as part of a conginetal heart complex such as tetralogy of Fallot or as a result of hypertrophic obstructive cardiomyopathy involving the right side of the heart.
Patients with pulmonary stenosis may live for extended periods completely without symptoms and frequently survive past the age of 70 years without surgical intervention, when they do occur, include tachypnea, syncope, angina or hepatomegaly and peripheral edema.
Pulmonary stenosis
Pulmonary stenosis can be valvular, subvalvular or supravalvular. Valvular pulmonary stenosis is the most common, accounting for 90% cases.
Subvalvular pulmonary stenosis can occur as part of a conginetal heart complex such as tetralogy of Fallot or as a result of hypertrophic obstructive cardiomyopathy involving the right side of the heart.
Patients with pulmonary stenosis may live for extended periods completely without symptoms and frequently survive past the age of 70 years without surgical intervention, when they do occur, include tachypnea, syncope, angina or hepatomegaly and peripheral edema.
Pulmonary stenosis
Monday, December 24, 2012
Arteriosclerosis and heart disease
What is arteriosclerosis? Arteriosclerosis is literally means hardening of the arteries, includes all kinds of diseases that damage the arteries and eventfully lead to coronary artery diseases. It involving arteries of various sizes and different layers of the arterial walls.
Arteriosclerosis is responsible for most of the deaths resulting from heart attacks.
The arterials diseases begins with damage to cells of the heart’s arteries and lead to the formation of a fibrous, fatty deposit called plaque.
The arterial plaque slowly increases in size until eventually the amount of blood flowing through the artery is greatly reduced or completely blocked.
If the coronary arteries that carry oxygen and nutrients to the heart muscle become obstructed , the flow of blood is cut off completely and a heart attack, or myocardial infarction, can occur resulting damage to the heart muscle.
Arteriosclerosis is the most prevalent chronic among senior citizens and the number one killer in the United States. It mostly affects those between the ages of 40 to 70.
Arteriosclerosis and heart disease
Arteriosclerosis is responsible for most of the deaths resulting from heart attacks.
The arterials diseases begins with damage to cells of the heart’s arteries and lead to the formation of a fibrous, fatty deposit called plaque.
The arterial plaque slowly increases in size until eventually the amount of blood flowing through the artery is greatly reduced or completely blocked.
If the coronary arteries that carry oxygen and nutrients to the heart muscle become obstructed , the flow of blood is cut off completely and a heart attack, or myocardial infarction, can occur resulting damage to the heart muscle.
Arteriosclerosis is the most prevalent chronic among senior citizens and the number one killer in the United States. It mostly affects those between the ages of 40 to 70.
Arteriosclerosis and heart disease
Subscribe to:
Posts (Atom)
The most popular articles
-
Aortic coarctation is a congenital heart defect marked by the narrowing of the aorta, typically near the ductus arteriosus just past the bra...
-
Peripheral Artery Disease (PAD) is a prevalent yet underdiagnosed circulatory condition where narrowed arteries impair blood flow to the ex...
-
Cardiovascular disease is a general term that includes heart attacks, heart failure, stroke and peripheral artery diseases. The term cardi...
-
Atherosclerosis is a pervasive and progressive disease primarily affecting medium-sized arteries, with significant clinical manifestations i...
-
Managing lipid levels in the blood is crucial for maintaining cardiovascular health, as high cholesterol and triglyceride levels can lead t...